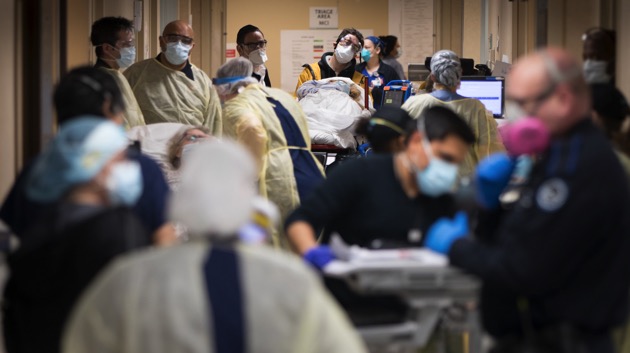
US hospitals strained with influx of patients amid latest COVID-19 surge, staffing shortages
Jeffrey Basinger/Newsday via Getty Images
(NEW YORK) — Explosive COVID-19 surge strains hospitals and schools around the nation
The number of hospitalized Americans who are positive for COVID-19 soared to more than 138,000.
For nearly two years, day after day, under exhausting and often dangerous conditions, health care workers across the country have continued to care for the nation’s sickest Americans who have fallen victim to coronavirus.
As the highly infectious omicron sweeps through the country, the United States is now facing its most significant coronavirus infection surge to date, putting additional pressure on an overtaxed health care system.
“We have seen an incredible proliferation of the virus in hospitals, such that we went from a place where virtually no county in the country was at risk of exceeding its capacity to well over half are now. I don’t like to make predictions, but things could get very bad in the coming couple of weeks,” Dr. Jeremy Faust, an emergency physician at Brigham and Women’s Hospital in Boston, told ABC News.
Although preliminary global studies indicate that the omicron variant may cause less severe illness than prior variants, health officials say that the sheer numbers of infections caused by the new variant could still overwhelm the health care system.
The burden on the health care system is made worse by nationwide staffing shortages and hospital capacity at elevated levels as many other patients seek care for non-virus related reasons.
“Due to the tsunami of omicron cases, the volume is affecting our health and community service,” said Dr. Rebecca Weintraub, assistant professor of Global Health and Social Medicine at Harvard Medical School. “While we are very lucky hospitalizations have decoupled, the vast spread is alarming.”
Late last month, Dr. Anthony Fauci, chief medical adviser to the White House, pointed to the disparity between cases and hospitalization as a “strong” indicator that omicron is less severe, as the U.S. has not experienced a concomitant increase in the relative percentage of hospitalizations.
Even so, Fauci warned that there will still be many virus-positive Americans who will seek medical care, creating further strain on hospitals.
“Even if you have a less of a percentage of severity, when you have multi-multi-multi-fold more people getting infected, the net amount is you’re still going to get a lot of people that are going to be needing hospitalization. And that’s the reason why we’re concerned about stressing and straining the hospital system,” Fauci told ABC News’ George Stephanopoulos during an appearance on This Week, earlier this month.
Experts say the baseline for hospitalizations is already higher than it was a year ago, with hospitals described by some experts as “relatively quiet” last winter for ailments other than COVID-19, which provided a “much bigger buffer zone,” to care for the most critically ill. In addition, hospitals were already struggling with patients from the delta wave.
“We entered this wave, with hospitals at a higher capacity than they were in previous waves, from non-COVID [health issues],” Faust explained. “That’s the real problem.”
Highly localized surges a pain point for many communities
An ABC News analysis of federal data found that in recent weeks, total hospitalizations — COVID-19 and non-COVID-19 related — have seen an uptick. The number of COVID-19-positive Americans who are hospitalized is now nearing a pandemic high, with more than 138,000 Americans hospitalized, and an average of 17,000 being admitted to hospitals each day.
Most of the patients who are requiring intensive care are still unvaccinated, according to top health officials, including U.S. Centers for Disease Control and Prevention Director Rochelle Walensky.
Experts say there is no overarching experience for how COVID-19 is now affecting the country, as surges are asymmetric, and the impact of COVID-19 will look different for every community.
“Ground conditions matter beyond belief,” Faust said, explaining that while one area can see an uptick in COVID-19 infections, hospitals may not become overwhelmed, because they have adequate staffing or a highly vaccinated and younger population, hospitals in other areas with lower vaccination rates and fewer resources could find themselves completely overwhelmed.
“There are places where incidental infection is a higher proportion of admissions than others. The reverse is true in other areas. And there are places with higher vaccination rates than others. When an unvaccinated person gets admitted to the hospital, they are going to be sicker and require more care and take up more resources. Every place is different,” Faust added.
Even within a state, the timing of surges is also highly localized, experts say, varying by areas and even by hospital. Thus, even if hospital capacity nationwide or on the state level looks relatively stable, “micro surges,” seen in individual facilities or communities may still be occurring and threatening care.
Even virus-positive patients who are not admitted primarily for COVID-19 are adding a strain
Nationwide, it remains unclear as to how many patients are being admitted to the hospital for coronavirus-related care, and how many patients are coincidentally tested positive for the virus, after they were admitted for other reasons and subsequently checked for positivity as a routine check.
In New York, state officials reported on Friday that 42% of COVID patients were admitted for non-COVID reasons, and in Florida, Gov. Ron DeSantis cited data from three of the state’s major hospitals, which reported that half, or more, of their COVID-19 positive patients are getting treated for other conditions, not the virus.
However, some experts and hospital officials have cautioned that the proportion of patients seeking care specifically for COVID-19 likely varies widely community by community. In addition, health officials say a COVID-19 diagnosis can cause additional strain on a health system, as virus-positive patients in many hospitals are required to be treated differently.
In a series of tweets last week, Dr. Ashish Jha, dean of the Brown University School of Public Health, stressed that both patients “with COVID-19” and those admitted “for COVID-19,” have an impact on care, utilization, and can stress the health care system.
Patients, who may have come in for another ailment, such as a broken leg, and are found to be positive for the virus must stay in a COVID-19 isolation room, explained Jha, who added that there are already a limited number of such rooms available.
In addition, every time a health care worker enters a room with a COVID-19 positive patient, they must be wearing full PPE, which in turn, prolongs wait times for many patients.
“Admissions with COVID is still very disruptive to the health care system, at a time when it can’t afford more disruption,” Jha said.
Federal data shows the emergency department visits with diagnosed COVID-19 cases are currently at their highest point of the pandemic — a figure that has more than doubled over the last month.
“People are in the ER for hours and days, creating gridlock for new patients that need emergency services every day,” said Dr. Jay Bhatt, an internist and adjunct faculty at the UIC School of Public Health and an ABC News Med Unit contributor.
Other hospital officials have noted that even if patients are admitted for a reason other than COVID-19, a COVID-19 infection on top of another condition may only exacerbate an individual’s original illness.
At Cincinnati Children’s Hospital Medical Center, hospital officials told ABC News that they have seen their COVID-19 positive patient totals “skyrocket” in recent weeks. Some of these patients happen to test positive while admitted for other concerns, while others are primarily sick with COVID-19.
“Even the children who are not admitted primarily for COVID have hospital courses that are further complicated because of COVID. Having cancer, heart issues, appendicitis, and COVID is never a good thing,” one hospital representative said.
A growing shortage of hospital staff ‘wreaking havoc’ on the health care system
Surge after surge, nurses, doctors and respiratory technicians have led the fight against the virus, many forced to leave their families for weeks to months at a time in order to avoid a total collapse of the health care system during the pandemic.
Since the onset of the pandemic, the already existing staffing shortage has only grown worse, and now experts say they are concerned there will not be enough front-line workers to care for the influx of patients in need as many of them are forced into isolation and quarantine after testing positive.
“I am worried we don’t have enough health care workers to care for patients flooding hospitals,” said Bhatt. “[The] unprecedented numbers of sick clinical staff [are] wreaking havoc on hospitals and health systems as they do their best to care for patients in this current surge. I have not seen a workforce issue as serious as this, and is deeply concerning.”
As of January 2022, there have been at least 819,000 coronavirus cases among health care personnel, and more than 3,100 virus-related deaths.
Late last month, the CDC shortened the isolation time for COVID-19-positive health care workers in anticipation of the potential shortages that might occur amid the latest surge.
Many health care workers say they are exhausted as they train to keep their facilities running.
“There are wait times in the emergency department that are running six to eight hours, in the trauma center. [In the] emergency room sometimes it runs greater than 24 hours. So you know we … the nursing staff is tired, we have burned out. We’re working 12- to 14-hour shifts, on Sundays up to 16-hour shifts,” Thomas Mapplebeck, a nurse in the Emergency Department at Baystate Health told ABC News.
Staffing shortages are also preventing some people from receiving the critical care they need, added Bhatt, who said that some patients in need of hospice are struggling to receive placement because of the shortages.
The unknown of what’s to come
Many health officials and experts have tried to forecast what Americans can expect from the virus in the months and weeks to come, and when COVID-19 will finally enter an endemic phase. However, Faust explained he is reluctant to make predictions as there is still so much unknown surrounding the virus.
“Five weeks ago, we’d never heard about omicron because it didn’t exist as far as we know, and now we were in the worst part of this pandemic,” Faust said.
With many younger Americans becoming infected, Faust said it is possible intenstive care unit bed capacity may not be overrun. It is also possible the virus could reach the millions of Americans who are still unvaccinated, as well as many at-risk people who remain vulnerable for severe illness.
An additional roadblock for some hospitals has been delays in returning patients to nursing rooms, further exacerbating the shortage of beds.
“Patients who are ready for discharge are having trouble getting back to long-term care, nursing home facilities, short-term rehab and home without social support as resources are strained and this creates a logjam that strains the system and workforce even further,” Bhatt said. “We can’t have situations where we are having trouble getting patients back to the community so that others that really need hospital care can get it. We can and need to do better.”
The worst-case scenario, said Faust, will be if nursing homes see significant spikes.
“If that happens in places that are already on the edge, we will see horrifying scenes that we’ve been warning against for a long time,” Faust said.
Health officials have stressed it will be critical for Americans to modify their behavior by wearing masks, avoiding mass gatherings and getting vaccinated.
“I hope people can do their part to get vaccinated, decrease the number of people who need hospital beds so that these other folks who are really sick have a chance to get the care that they need,” said Dr. Jeff Pothof, an emergency medicine physician at UW Health in Madison Wisconsin. “It’s really bad right now,” he added.
Benjamin Rader, a research fellow at Boston Children’s Hospital, contributed to this report.
Copyright © 2022, ABC Audio. All rights reserved.